Jackie Yencha hit the wall at age 22. “I couldn’t handle the pain any more,” she says. “I was terribly fatigued, not feeling well, not sleeping well.” But it took Yencha seven years to get an accurate diagnosis of fibromyalgia.
Her first diagnosis — reflex sympathetic dystrophy — resulted in experimental surgery that did nothing to relieve her pain. In fact, numerous surgeries followed to correct the problems from that procedure. Years went by. Yencha was still in pain, still getting little sleep.
“I became desperate … the pain never got better,” Yencha tells WebMD. That’s when she headed to the Cleveland Clinic, where comprehensive testing showed she had fibromyalgia.
“You need to find a doctor who will listen and who really knows fibromyalgia,” says Yencha.
“A lot of doctors out there don’t know much about it,” she explains. “We hear from people all the time … people in small towns who say no one here has ever heard of this.”
What Is Fibromyalgia?
Fibromyalgia is a chronic condition that causes disabling pain all over the body — as well as stiffness and tenderness in muscles, tendons, and joints, experts say. It is most common among women ages 35 to 55.
Although it’s one of the most common muscle problems, the cause is a mystery, fibromyalgia researchers say. There is no inflammation or joint damage, as occurs with arthritis. There is no damage to internal body organs, as with rheumatoid conditions like lupus. It is called fibromyalgia syndrome because it is identified by a collection of symptoms.
Indeed, the list of possible fibromyalgia symptoms is a long one:
- Chronic muscle pain
- Muscle spasms or leg cramps
- Sleep problems
- Severe fatigue
- Anxiety
- Depression
- Morning stiffness
- Headaches
- Difficulty concentrating
- Skin sensitivities
- Irritability
- Intestinal problems
But these are also common to liver disease, lupus, Lyme disease, thyroid dysfunction, heart disease, arthritis, degenerative joint disease, chronic fatigue syndrome, irritable bowel syndrome, and other disorders — and therein lies the difficulty in diagnosing fibromyalgia.
How fibromyalgia develops is also a mystery. “The onset can be fairly abrupt, triggered by a motor vehicle accident or a mishap at work,” says Steven Berney, MD, chief of rheumatology at Temple University Health System in Philadelphia. “Very quickly the condition sets in. You feel bruised for the next couple of days, but there’s the expectation that whatever is disrupted will heal. When the pain doesn’t wear off, it becomes clear something else is going on.”
More typically, there is a gradual onset, Berney tells WebMD. “The pain becomes more severe over time. That’s more difficult to diagnose. You’re looking for something that set this off, and you can’t find it.”
Fibromyalgia research shows that the disorder seems to run in families. Recent studies show that genetic factors may predispose some people to fibromyalgia. An illness or injury that causes trauma to the body can make subtle fibromyalgia symptoms more apparent — and more troublesome, according to the National Fibromyalgia Association.
“The pain is very real and markedly impedes their lives,” Berney says. “People who were very active become disabled by pain and fatigue. ‘I want my life back’ becomes the charge.”
The Tender Points of Pain With Fibromyalgia
While it’s not clear what exactly triggers fibromyalgia, researchers are homing in on the basic mechanisms. Fibromyalgia is considered a disorder of pain regulation. Patients have higher levels of two substances — a nerve chemical called substance P, and nerve growth factor in the spinal fluid. They also have lower than normal levels of the brain chemical serotonin, as is also true with people suffering from depression and anxiety.
All this produces a dysfunction in the body’s ability to process pain — and creates supersensitive nerves throughout the body, explains Andrew J. Holman, MD, a rheumatology specialist at the University of Washington in Seattle. To make things worse, people with fibromyalgia have difficulty getting a good night’s sleep — so they constantly wake up feeling fatigued.
The result: Everyday sensations of discomfort and pain are amplified beyond the norm. Slight bumps and touches can cause disabling pain if you have fibromyalgia. This pain can be aggravated by outside factors — noise, weather changes, and stress.
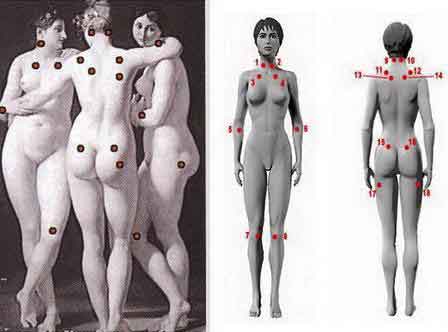
To figure out what’s going on, doctors diagnose fibromyalgia by examining specific “tender points” on the body. “There are 18 specific tender points — specific locations that are tender for everyone,” Holman tells WebMD. “But for people with fibromyalgia, these points are significantly more tender. People are more sensitive at those points. A dysfunction in the central pain processing amplifies their sensations.”
Tenderness or pain in at least 11 of these 18 points is the hallmark of fibromyalgia, says Holman. Also, the pain is widespread on both sides of the body — neck, buttocks, shoulders, arms, upper back, and chest. Tender points are around the elbows, shoulders, knees, hips, back of the head, and the breast bone.
Doctors test these tender points to make the fibromyalgia diagnosis. Yet it’s not always so clear-cut what the widespread pain indicates. It takes a careful ear to discern what’s really going on, explains Martin Grabois, MD, chairman of physical medicine and rehabilitation at Baylor College of Medicine in Houston.
“Physicians are used to diagnoses like a herniated disc, where there’s pain in a specific location,” Grabois tells WebMD. “That’s not so with fibromyalgia. Some pain is above the waist, some below the waist, at the shoulders, etc., and there are sleep disturbances, fatigue. These are symptoms of a number of diseases. They are not isolated to fibromyalgia.”
The muscle pain can range from mild discomfort to severe enough that it limits a person’s everyday life — including work and social activities. The pain is often described as burning, gnawing, throbbing, stabbing, or aching. When the person relaxes, the pain may be more noticeable — and less so when they’re active.
Originally posted 2023-04-07 11:06:21.

